Gentle Procedures Dallas is committed to providing an affordable, quality vasectomy surgery. We offer the no-scalpel, no-needle, open-ended vasectomy procedure to all our patients.
The cash-pay price for a one-time visit to the clinic for a consultation and vasectomy is $730. There is a $100 scheduling fee to book the appointment. The balance of $630 is due at the time of service. We keep our pricing reasonable so that our high-quality procedure can be affordable to all.
Dr. McAuliff keeps his fees low so the procedure can be affordable to everyone. He offers you “concierge” type care. You will be given his personal cell phone number at the end of the surgery and you will be able to text or call him personally with any post-operative concerns or questions. The staffs’ goal is to give personalized service by giving you as much time as it takes to answer your questions. We will work with you to provide you with the tailored services you need. Instead of requiring two visits to the office as many physicians require—one visit for the surgery consultation and a second visit for the surgery—Dr. McAuliff tries to be respectful of your time by offering only one visit to the office, making it more convenient for you.
QUESTIONS? READY TO GET STARTED?
Call: 469-931-0684 or fill out the form below.
No-Needle Anesthesia is Always Included
Dr. McAuliff employs the no-needle anesthesia, no-scalpel procedure for all vasectomies.
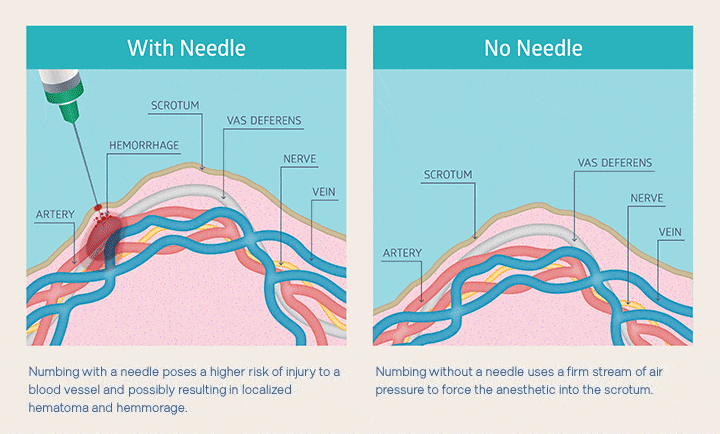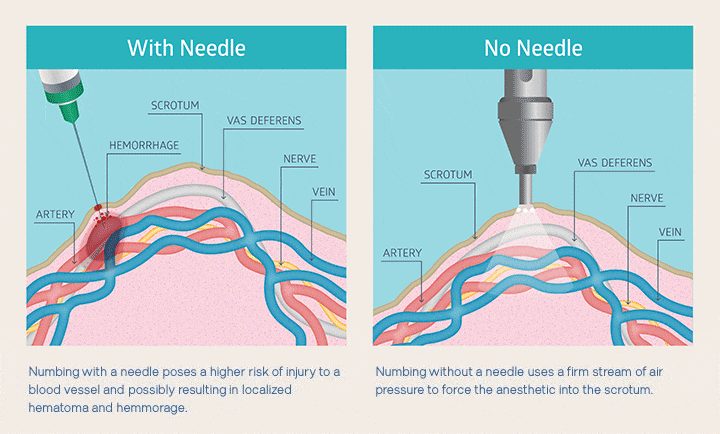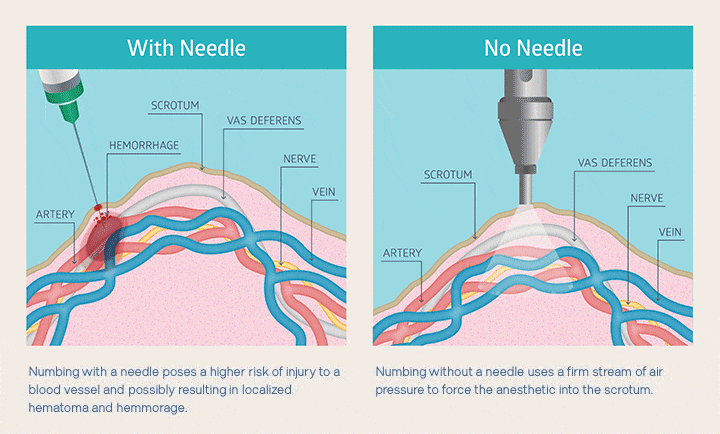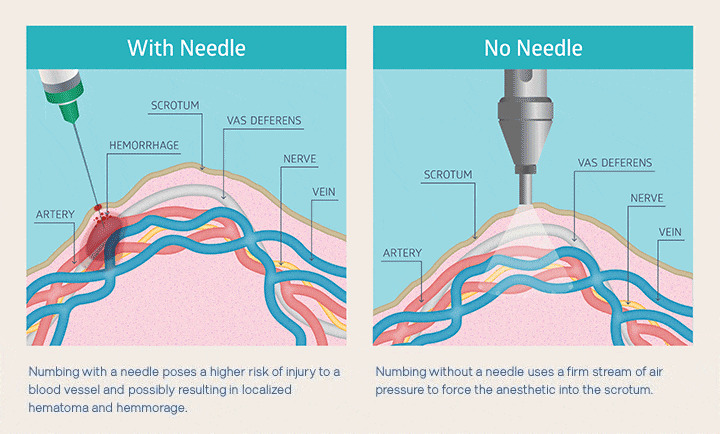
Nobody likes a needle in the scrotum, so no-needle anesthesia is pretty much universally preferred. You can see below how the air-jet anesthetic application reduces trauma compared to injection using a needle.
Vasectomy Fees & Paying For Your Vasectomy
When you schedule your procedure, there is a $100.00 non-refundable scheduling fee to book the appointment, which is applied to the cost of the surgery on the day of the procedure. The remaining $630 is due the day you have the vasectomy done. Please understand that the $100 booking fee is non-refundable under any circumstances.
Paying for Your Vasectomy
The cash price for a vasectomy is $730. That includes your initial consultation with the doctor, the procedure, and any post-surgery support during the healing process.
More Efficient Process
The staff at Gentle Procedures Dallas work together like a well-oiled machine. The clinic staff are conscious of getting you in right on time, no waiting. The process is orchestrated from start to finish to make it as easy as possible on you. If you wish, Dr. McAuliff can prescribe a mild sedative for you to take immediately prior to the procedure to calm your nerves. If you do take this medication, you will need to have a driver bring you to the clinic and take you home afterward.
Upon leaving, you will receive a post-procedure packet that has all the answers to the questions you didn’t think to ask, such as expected bruising, healing time, when you can go back to performing given tasks, what to look out for, and when to call.
Cancellation Policy
The $100 fee to book your appointment is non-refundable under any circumstances. We have this policy for a couple of reasons.
We have this policy to help you to follow through on your decision for a vasectomy. Many men have vivid imaginations of what the procedure will entail and might even back out of their appointment except that the non-refundable $100 scheduling fee keeps them accountable to their appointment.

We also employ this policy out of consideration for other clients who might have wanted to schedule in the time slot that has your name on it, but they couldn’t because it was being held for you. If you back out, they didn’t have the chance to choose that date and time.
The $100 fee to book your appointment is non-refundable BUT if you cancel and reschedule 7 calendar days or more before the date of your appointment, the $100 booking fee that you paid can be applied to reserving the new appointment and will roll into the cost of the procedure on the date of the new appointment.
When you book your appointment and pay the $100, think of it as purchasing a surgery time slot that no one else can have. If you cancel, you give up your $100. If you decide to cancel 6 calendar days or less before the date of your appointment, even if you wish to reschedule, the $100 scheduling fee will not apply to the cost of the new scheduling fee for the new appointment because of the late date of your cancellation. In this case, you will need to pay another $100 scheduling fee if you wish to book a new appointment time.
Any time that you cancel and don’t reschedule or that you decide to be a no-show, you forfeit the $100 fee you paid for the appointment time. This policy is in place to encourage you to be certain that you are serious about scheduling an appointment for the procedure.
Please call us at 469-931-0684 to confirm your appointment for a no-needle, no-scalpel vasectomy.
We are available by phone during regular clinic hours, 9-5, Monday through Friday, and this is the best way to reach us for quick questions and appointments.
We offer the option of a single visit for consultation and procedure because that is what most men seem to want.
Can I Use My Insurance
We don’t take insurance because insurance companies won’t let us practice medicine the way we want to do it. We want to be able to offer a vasectomy procedure in a single visit and insurance companies won’t reimburse unless we require our patients to come at least 3 or 4 times to the clinic. Most insurance plans will require that you make an appointment one day for a pre-surgery consultation, a second day for the surgery, and a third day for a follow-up. Then they require you to come back to the clinic for a semen sample. By not taking insurance, we can offer you the convenience of taking off from work for only one day.
We offer a cash price of $730 and a single visit to the clinic. If you have health insurance and you believe it might cover part of the expense of a vasectomy, your insurance company can walk you through the process of filing an out-of-network claim and we also have detailed instructions—just mention to us that you would like to receive printed instruction and a detailed receipt. When you are ready to file, call the number on the back of your insurance card. Your particular insurance policy will determine whether or not the policy will cover some of the expense. Any reimbursement of your cost will be between you and your insurance company. We will not remain involved to receive any of the insurance reimbursement because you have already paid us in full.
Here’s how it works at our clinic: We collect a non-refundable $100 from you to book the time slot and then the $630 balance for the procedure is due on the day of the surgery for a total cash price of $730.
At Gentle Procedures, $730 is all you will pay for your vasectomy with the advantage of the no-needle, no-scalpel, open-ended technique and faster recovery, in-and-out of the clinic in less than an hour. If you want the best service and the most comfortable procedure possible, it’s a price worth paying.
If you’re thinking, “But I want to use my insurance”, when you start to looking at the numbers if you choose another provider, you may be surprised to find there is no advantage to using your insurance for your vasectomy. That’s because, if you were to go to another provider who charges more but takes insurance, your out-of-pocket cost required by your insurance policy might end up being the same as our cash price. Your insurance carrier determines your portion of the responsibility, and often, with copay, co-insurance, and deductible, the patient portion comes out being about the same as our $730 cash price.
If you want the convenience of a single visit to have the procedure done by the no-scalpel, no needle method, by a physician who specializes in vasectomies, ours is a price worth paying. Look at it this way – $730 is less than the price of a new set of tires for your car and it’s only a one-time expense! Or it’s about the price of a week’s worth of groceries for a family of 4.
Why Don’t We Accept Health Insurance?
It’s not easy for a small, independent clinic to deal with insurance companies. Most people do not realize that insurance pays about 50 cents on the dollar charged or doesn’t pay at all or takes back the payment months later. That makes it very difficult for independent medical practices to remain viable.
It has been our long experience that, prior to the surgery, health insurance companies often provide inaccurate information regarding an individual’s coverage for a procedure and how much a patient may owe. After the procedure has been completed, it is not unusual for health insurance companies to inform the physician that the information they provided during pre-verification was inaccurate. For example, prior to the surgery, it is not unusual for the agent to say a person is fully covered and give us a specific amount he has to pay. Several weeks after the procedure, the insurance company will then tell us they made a mistake, the procedure was not covered and the patient needs to pay more co-insurance.
Our office is then put in the awkward position of having to contact the patient and ask for more money. By then, our patients are long-gone and often these calls are not well received. We end up in the middle of the patient and his health insurance company and the health insurance companies try to distance themselves from the problem they caused because their staff provided inaccurate information. In this scenario, when we send the patient a statement, because the surgery is a “one-and-done” procedure and we never see the patient again, the patients often simply ignore the statements we send. Our office is then required to take the loss…even though we had nothing to do with the confusion.
We consistently have good reviews from patients. When we do have dissatisfied patients, it is because their health insurance company has provided inaccurate information and we had to become “the bad guy” to try and collect payment from the patient who believes we are being unfair. These patients often unfairly blame our office for the mistakes or delays by their health insurance company.
If You Want To Use Your Health Insurance
If you have health insurance and you want to use it, it's not that complicated to file your own insurance claim. In fact, because you are the customer and we are not, the insurance companies often deal more quickly with you, the policy holder than they would with us. If you want to file a claim, we will give you extensive instructions for how to file a claim for an out-of-network provider. If you call the phone number on the back of your insurance card, a representative can also walk you through the process.
If your policy does cover the procedure and if your insurance company does have a reimbursement, that money will come directly to you and not to us as a billing provider.
Call Us to Book!
469-931-0684
REQUEST A VASECTOMY APPOINTMENT
Better outcome
Dr. McAuliff focuses on performing only a few out-patient surgical procedures. This means you’re getting a physician who is well-experienced in doing vasectomies. A doctor who practices doing a procedure over and over often experiences better outcomes than a doctor who does a vasectomy only occasionally while having much of his time devoted to a wide spectrum of other procedures.

Greater concern for your well-being
Your comfort is our greatest concern at Gentle Procedures Dallas. We know that our patients are nervous when they come in but we try to alleviate that. You will be awake during the procedure but our goal is that you feel no pain. The doctor starts with a numbing spray, followed by an anesthetic which some men describe as a “pinching” feeling but very minor, then you won’t feel anything during the rest of the procedure. During the procedure, Dr. McAuliff enjoys conversing with his patients. He likes to use this time to get to know his patients, what they do, and where they’re from. As he works, Dr. McAuliff will provide a lot of general advice for best healing.
It’s our goal to hold your hand during the entire process, so you will be at ease and well-informed. This is the measure of care that you will receive from our entire staff.
Does that sound like the kind of service you want to receive for only $730? For the top-level service you deserve, give us a call 469-931-0684.
Call Us to Book!
469-931-0684
